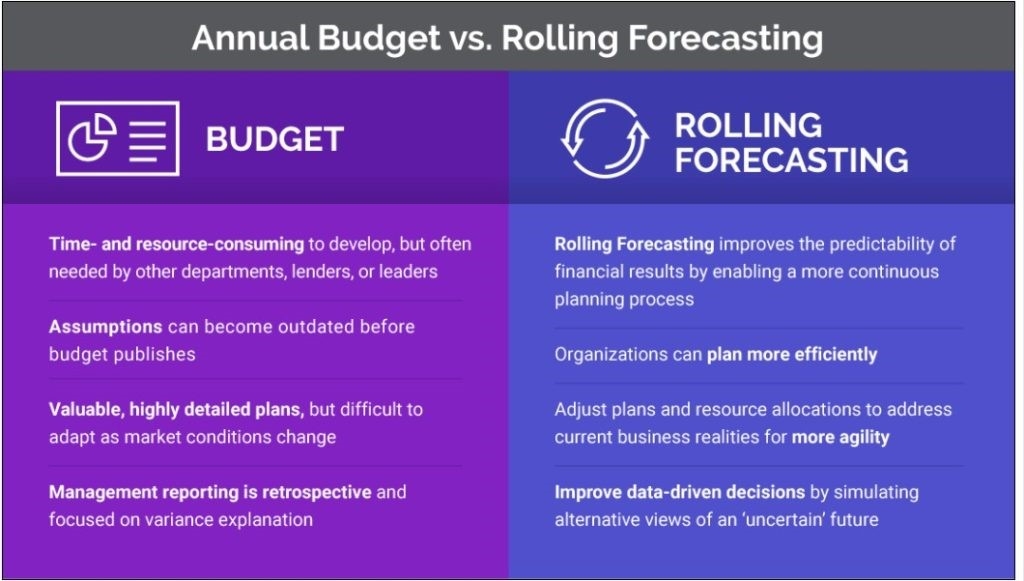
Following the initial pandemic shutdowns in spring 2020, interest skyrocketed in rolling forecasting to either complement or replace annual budgeting — and with good reason.
Once a budget is created and approved, it begins degrading in usefulness as internal and external forces on a budget constantly change. In contrast, rolling forecasting is the process of reexamining financial information on a regular cadence to provide timely visibility into changing financials.
A survey of healthcare executives in fall 2020 showed that 12% of respondents use rolling forecasts instead of annual budgeting, nearly double from 7% in 2019. Nearly half (49%) use rolling forecasts to complement annual budgeting, and nearly 60% indicated their organizations would make rolling forecasting a priority.
Because rolling forecasting works by regularly reviewing and adapting to financial information and annual budgets make a point-in-time determination to help with planning, both methods play important roles that benefit healthcare organizations and empower finance teams.
Annual Budgets Versus Rolling Forecasting
Annual budgets are useful in setting the plan for the upcoming year but are generally time-consuming to produce — nearly 50% of healthcare organizations spend six months or longer preparing them. Developing budgets for next year will likely still be necessary for most organizations because these documents guide departmental financial plans and are often required by lenders or leadership.
Rolling forecasting enables healthcare leaders to update their financial projections on a monthly or quarterly basis to determine, “How has the previous month or quarter changed our view of the present and future?” It guides informed course corrections in response to current data and helps update near- and long-term projections. Rolling forecasting influences not only current expenditures and initiatives — such as ramping up traditional services at a time when consumers may avoid returning to a hospital setting — but also strategic decisions and future endeavors.
The agility and visibility that rolling forecasting provides help healthcare leaders adjust strategy quickly as financial conditions change.
How Rolling Forecasting Works in Healthcare
Here’s how rolling forecasting works:
- Budget process participants come together for short blocks of time each month or quarter to assess and update the organization’s financial performance.
- Participants select the appropriate forecast horizon (e.g., monthly or quarterly periodic forecasts for the current year and up to two years forward).
- Comparative and trend analyses are performed using the most recent data available, often taking multiple scenarios into account. For example, organizations typically test against at least three sets of conditions to analyze the forecast for sensitivity and risk, with favorable, unfavorable, and very unfavorable outlooks.
- Based on these analyses, leaders evaluate key actions their organization should take now and in the short- and long-term to strengthen and protect performance.
Most healthcare organizations use rolling forecasting to create forecasts for six to 12 quarters — a longer time horizon than used for current-year forecasting or traditional healthcare budgeting processes.
Scripps Health, a nonprofit health system based in San Diego, has used quarterly rolling forecasts for a few years, and those forecasts proved valuable during the pandemic to shape Scripps Health's response to patient volume shifts.
For example, the system runs daily reports that monitor charges and productive hours to track the impact of reduced elective procedures and the corresponding flexed labor. Because these decisions are made differently at each of five hospitals, rolling forecasting helps leadership understand the impact by location and department — showing which departments are flexing properly and where volumes are dropping. This has helped guide decisions such as when to temporarily close specific clinic sites and departments and which resources to repurpose in the event of a surge.
When Scripps’ daily charges report showed a 35%-37% drop in volume, finance leaders began analyzing the revenue impact over a two-week period and projecting volumes quarterly. As volumes picked up, daily analyses helped make staffing and supply adjustments, with an eye toward patient acuity levels.
As Scripps Health began its return to elective procedures, rolling forecasting also informed which departments to open for service and how to adjust staffing for anticipated versus actual volumes. Ultimately, the cost data captured also supported the health system’s efforts to secure federal dollars for pandemic response, such as funds available through the CARES Act.
Each quarter, Scripps Health’s finance team makes process improvements to expedite decision-making, especially during this period of volatility. They strive to improve every quarter — prioritizing the time to think strategically and critically about issues and not allowing themselves to be solely driven by a specific deadline. John F. Wong, Scripps Health’s Director of Corporate Financial Planning and Reporting, has stated that rolling forecasting empowers his health system to make the right decisions in a changing environment — which is precisely why healthcare organizations need rolling forecasting now more than ever.
Axiom™ Enterprise Planning integrates rolling forecasts with long-term financial plans and operational budgets to support strategic and tactical planning success, comparing forecasts to established targets and key performance indicators.
You Might Also Be Interested In...

5 Approaches to Effective Budgeting and Forecasting in Healthcare

Scenario Planning for the Agile Healthcare Organization