What is healthcare benchmarking?
Healthcare benchmarking is the process of comparing one hospital, department, service line, provider group, or other dimension with another for the purpose of quality improvement. By understanding the hospital benchmarking data for one particular measure, a hospital can determine where it stands in relation to peer organizations and undertake an improvement initiative, if necessary.
Quality improvement projects could result in higher profits, lower hospital readmissions or hospital-acquired infections, higher physician productivity, or lower labor or supply costs per adjusted discharge. Every hospital has its unique strengths and weaknesses, so the types of improvement efforts will vary by facility.
How are benchmarks used in healthcare?
Benchmarking in healthcare allows hospitals to compare themselves to best-in-class facilities, hospitals with similar attributes such as bed size, and hospitals in their local or regional area. It also allows hospitals to determine how they stack up against other providers on standards set by the Centers for Medicare and Medicaid Services (CMS) and other regulatory agencies.
Healthcare benchmarking datasets include:
- Hospital data. On a hospital level, benchmarking encompasses such macro metrics as revenues/expenses, volumes, margins, and non-operating liabilities and assets that demonstrate the overall health of the hospital.
- Physician data. Benchmarking data can compare physicians individually, by department, or against other departments locally, regionally, or nationally. For physicians within a department, for example, once top-performing physicians are identified, data on individual physicians can reveal performance improvement opportunities and specific areas where leaders should focus their attention.
- Nursing data. Using internal benchmarks, leaders can compare nursing departments against patient metrics such as length of stay, readmissions, labor costs per adjusted discharge, and more.
- Clinical analytics. Clinical analytics include any measure that impacts patient care. Data can tie cost savings to quality-of-care metrics to identify best practices, reduce unintended clinical variation, and quantify preventable complications, readmissions, and safety events.
Why is benchmarking in healthcare important?
Benchmarking is a critical tool to help organizational leaders make the right strategic choices, remove risk from decision-making, and defend the validity of actions/inactions through the effective use of data. Ultimately, the purpose of healthcare benchmarking is to improve efficiency, quality of care, outcomes, and the patient experience. To do this, financial, operational, and clinical benchmarks should be used throughout the organization to help pinpoint sources of concern and opportunities for growth.
The importance of different types of benchmarks
Financial benchmarks are important because they paint a picture of the financial health of the organization, such as your ability to leverage cash or credit positions. Operational benchmarks are important because they measure resource utilization. And finally, clinical benchmarks are important because they measure care outcomes. Different type of benchmarks are important for different audiences, but together, financial, operational, and clinical benchmarks give healthcare leaders, clinicians, and physicians a multi-dimensional view of performance that can help reduce costs, improve outcomes, and better serve the community.
What are the benefits of benchmarking in healthcare?
Healthcare benchmarking gives leaders the confidence to know the direction the market is moving and their position in relation to best-performing hospitals, peer hospitals, and local and regional competitors. Benchmarking data can identify how far a hospital needs to go to reach a particular goal, where competitors have an advantage, and where a hospital outpaces others.
What are the different types of healthcare benchmarking?
No hospital can be best in class on every measure, so benchmarking is a balancing act that begins with determining a baseline metric for a particular measure before embarking on any improvement initiative. Savvy hospitals start in areas with the most upside potential, such as cost savings, quality improvement, or revenue increases.
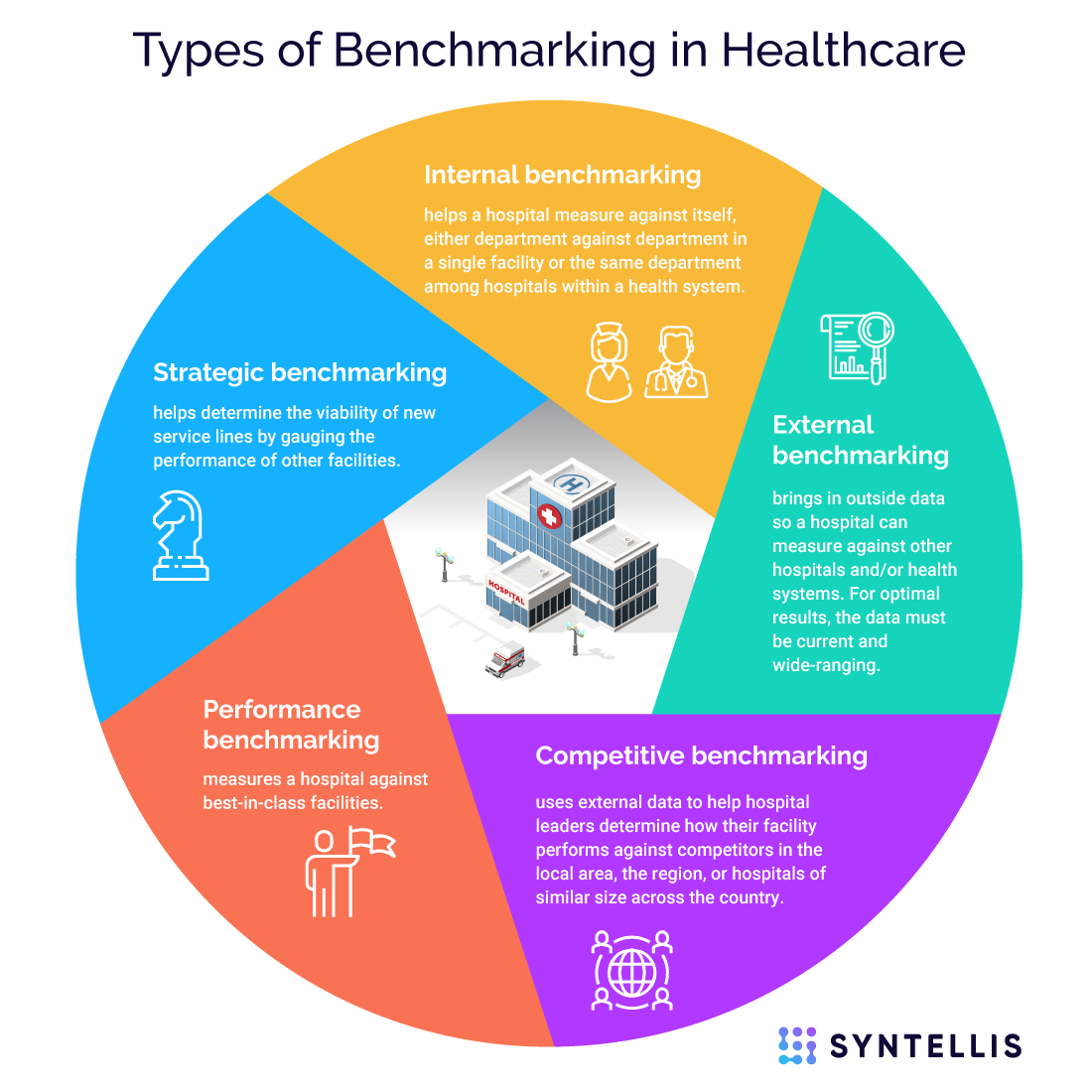
Types of benchmarking include:
- Internal benchmarking helps a hospital measure against itself, either department against department in a single facility or the same department among hospitals within a health system.
- External benchmarking brings in outside data so a hospital can measure against other hospitals and/or health systems. For optimal results, the data must be current and wide-ranging.
- Competitive benchmarking uses external data to help hospital leaders determine how their facility performs against competitors in the local area, the region, or hospitals of similar size across the country.
- Performance benchmarking measures a hospital against best-in-class facilities.
- Strategic benchmarking helps determine the viability of new service lines by gauging the performance of other facilities.
What are the challenges in benchmarking? How do leaders react?
The biggest challenges in hospital benchmarking include finding suitable external data sources and ensuring external data can be effectively integrated with internal data to produce meaningful comparisons.
Many hospital leaders believe their organizations are unique and beyond comparison. Within the world of benchmarking, however, the idea is not to find an exact match. Instead, organizations want multiple comparison groups that provide a range of metrics that show performance against internal benchmarks and help identify potential new performance opportunities.
Even hospitals in the top quartile of national or regional benchmarks cannot be complacent. Being at the highest performance level does not mean that the journey is over; it means less distance to travel.
What defines quality healthcare benchmarking data?
Healthcare leaders should look to the largest data sources — in terms of the number of hospitals, departments, and physicians — that are updated at least monthly. Quarterly data updates are not sufficient to capture true performance against static benchmarks. Also, is this a data source that you trust? Ask peer organizations about their data sources and look to healthcare consulting companies to see where their data comes from.
The power of benchmarking occurs when hospitals study how other organizations achieve top performance levels and then adapt those strategies for their own use.
How are benchmarks determined in healthcare? How do I set benchmark priorities?
Every hospital will have different healthcare benchmarking priorities based on its unique strengths and weaknesses. Healthcare benchmarks are determined by deciding which department or service line to focus on, establishing a baseline of performance in that area, and then finding peer information to see where you stand against similar hospitals. The first focus areas should be the ones where an improvement project would have the most significant impact (e.g., the low-hanging fruit).
As hospitals move from benchmarking as a comparison exercise toward benchmarking as a process to take them to best-practice status, keep these strategies in mind:
- Include key stakeholders in the entire process
- Use both internal and external lenses
- Look beyond nearby hospitals for comparisons
- Be aware of reporting time lags
- Avoid a one-size-fits-all approach
- View benchmarking as a way to motivate caregivers
List of healthcare industry financial & operational benchmarks
Hospital benchmarking can incorporate innumerable measures across every department, but at the executive level, these are the top hospital finance and operational benchmarks that should be tracked at different levels, including provider, department, hospital, and health system.
- Operating Margin: Measure profit after accounting for costs
- Volume: Track the output and utilization at all levels of the organization
- Revenue: Ensure incoming cash is sufficient to cover expenses and monitor changes in various revenue-producing areas
- Total Expense: Monitor total cost at various levels of the organization
- Labor Expense: Determine the percentage that labor contributes to total expense and monitor the composition of the labor expense
- Costs by Payer: Understand the types of health insurance your patients have and how that impacts your bottom line
- Physician Investment: Track how much your health system spends to subsidize physician practices
- Compensation: Evaluate whether you are over- or under-paying the position types within your organization, including physicians
- Productivity: Understand the output of each department, practice, and facility in relation to labor time and cost to produce that volume of output
Healthcare’s largest dataset, updated monthly
Axiom™ Comparative Analytics features the most robust and complete dataset in the industry, including data from more than 1,000 hospitals, 6,000 benchmarks, 135,000 physicians, 130 physician specialties, 350 departments, and 100 job classes updated each month.
External comparison data is refreshed monthly and available when month-end close concludes, providing healthcare providers with the industry’s most timely access to current financial analytics.
Features include:
- Metrics Explorer, with an interactive dashboard interface to view key performance indicators (KPIs) with drill-to-detail capabilities
- Data Explorer to compare data in a more traditional table structure to highlight variances and opportunities
- Performance Dashboards, with a proprietary algorithm, prioritizes and displays problem areas in context with budgets, trends, and peers

Discover what’s possible with Axiom Comparative Analytics
Independent analysis from Hobson & Company shows that Axiom Comparative Analytics delivers significant efficiencies and return on investment (ROI). The potential cost savings or revenue enhancements can be substantial. A Midwestern hospital with 200-299 beds saved $1.1 million by improving surgical productivity per equivalent patient day. A similar-sized hospital in the West saved $1.2 million by decreasing ICU spend per equivalent patient day by 12%.
Comparative Analytics uses a uniform classification process to compare data and eliminate the burdens of data normalization and submission, cutting by 50% the time spent on reconciling, loading, and normalizing data
Axiom Comparative Analytics brings actionable intelligence to hospital decision-making