For hospitals and health systems seeking to analyze financial performance, assess or set prices, or engage in more successful contract negotiations, understanding the underlying cost of healthcare products and services is essential. This costing knowledge brings informed decision-making at both the tactical and strategic levels and is vital to hospital and health systems’ cost containment efforts.
There are many methods of cost accounting in healthcare, but two higher effort, more advanced methodologies — activity-based costing and time-driven activity-based costing — have attracted growing interest. While these methods can provide meaningful analytics, for many organizations, the level of detail requires a heavy lift. A tiered approach to activity-based costing matches intensity of effort with potential impact on organizational performance and helps finance leaders identify when to use activity-based costing and when to opt for an easier method.
Understanding the Basics of Activity-Based Costing
But first, what is activity-based costing? Activity-based costing, sometimes called ABC or ABC costing, is a collection of tools that enable organizations to more precisely associate cost with each service or patient encounter. This costing method ensures that cost is assigned as it is incurred through activity measures. Time-driven ABC is a specific form of activity-based costing used to calculate the cost of time-based healthcare resources consumed, such as operating room utilization, as a patient moves through the care process.
Tracking these activities and costs allows the finance team to precisely assign the true cost of a service to the patient, thus creating very precise and reliable cost results.
Knowing the Limitations
Costing is an art, and there will always be some level of smoothing or averaging. The goal is to minimize this effect and assign true costs (i.e., vendor cost) where possible. With activity-based costing, the trick is to keep this view of patient cost aligned with the organization’s overall profitability view. Assigning cost based on anything other than the general ledger (GL) can lead to variances that may cause stakeholders to question the results. Addressing any deviation from the general ledger is warranted and will lead to more confidence in the costing data.
After all, the goal of a robust costing system is robust analytics. The analytics available for organizations that choose an activity-based approach to costing can help boost hospital finances through increased precision, even if some deviation from the GL occurs. Costing is truly a balance of art and science.
Establishing the Right Frequency
As finance leaders adopt more detailed costing methods, they should also consider the calculation frequency and the costing time period. A move from year-to-date to monthly or quarterly periodic costing will improve opportunities for trending. For many organizations, a quarterly processing cycle will strike the right balance between a timely refresh of costing data and demands on staff time.
When Should Activity-Based Costing be Used?
A modified approach to activity-based costing can balance an organization’s desire for operational excellence with its need for repeatable, low-maintenance solutions. Key to this approach is identifying areas in which the effort involved in activity-based costing will be rewarded with a significant impact on financial or clinical performance, operational efficiency, or organizational decision-making.
For example, as hospitals and health systems face downward pressure on payment rates and a push toward greater price transparency, finance leaders likely will need a more detailed understanding of the costs associated with individual patient encounters. A tiered approach to costing focuses the most intense efforts on high-impact items.
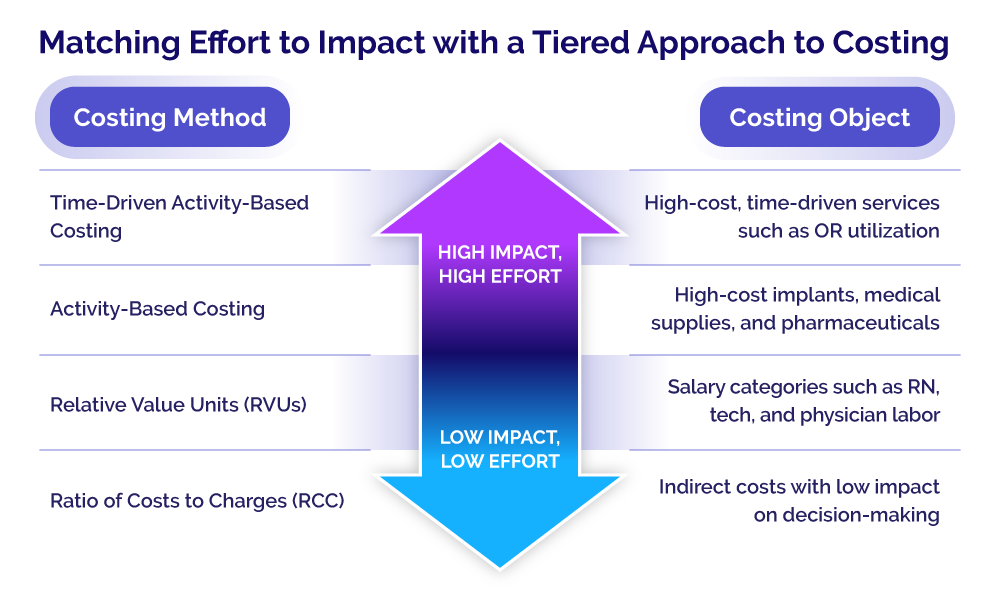
To better understand how to match effort with impact, consider a hip replacement surgery. Time-driven activity-based costing can be used for high-cost, time-driven activities such as surgical suite utilization, while activity-based costing should be used for high-cost implants, medical supplies, and pharmaceuticals. The assignment of actual vendor cost to the chargeable item, or even directly to the individual patient encounter, can provide valuable insight into the impact of physician preferences on the cost of an episode of care. Paired with data on clinical outcomes, these insights from activity-based costing can help identify which items produce the best outcomes at the lowest cost, ultimately helping to align cost with quality.
At the next level of intensity, relative value units (RVUs) can be used for staff salary expenses such as nursing, tech, and physician labor.
At the lowest intensity level, a traditional ratio of cost to charges (RCC) approach can be used to allocate expenses in areas such as non-chargeable supplies or miscellaneous costs that have a very low impact on decision-making.
The Impact on Indirect and Semi-Direct Costs
Activity-based costing may also generate value in areas that are not immediately apparent. For example, a more detailed approach to costing for areas of indirect or semi-direct costs can provide valuable insights into the true cost of patient encounters. At the same time, this helps mitigate the distortion of results that can occur when these costs are allocated solely based on statistics such as revenues, expenses, or FTEs.
Indirect expenses from areas such as surgery scheduling, cancer registry, patient financial services, and case management can be assigned based on the related clinical activity to individual patient encounters as direct, controllable costs. Similarly, semi-direct costs, such as clinical administration departments’ expenses, can be redirected to specific direct departments to facilitate full-cost assignment.
Benefits of a Tiered Approach to Activity-Based Costing
By focusing higher-intensity costing methods on high-impact areas, a modified activity-based costing approach drives efficiency and helps ensure stakeholders that their time is wisely spent on high-value efforts. Improved transparency of true costs helps establish confidence in the costing data.
As the benefits of a tiered activity-based costing approach become evident, finance leaders may decide to dedicate more resources to higher effort areas and less to those requiring lower levels of effort. Throughout this process, organizations will need a cost accounting solution that has the capability and flexibility to:
- Cost all components with the most appropriate methodology
- Enhance costing methodology for different components over time
- Pull these components together to present a full and accurate picture of the organization’s costs
By finding the proper balance between high- and low-effort costing areas, finance leaders can help put their organizations on the path to improved financial and clinical performance.
See how Axiom™ Enterprise Decision Support helps healthcare organizations modify activity-based costing practices to match effort with impact.